In a nation with effective Emergency Preparedness, a stitch in time can save countless lives when crisis strikes!!
Most health emergencies in Nigeria don’t begin in hospitals.
They begin at home, on the road, in offices, markets, churches, farms… ordinary places where ordinary people suddenly find themselves facing extraordinary situations.
A sudden collapse. A serious injury. A snakebite where antivenom is miles away. A child struggling to breathe. A loved one who suddenly becomes unresponsive.
In those moments, people don’t act based on policy documents or hospital protocols. They act on instinct, memory, and whatever knowledge they already have. That is why emergency preparedness is not something that starts when an ambulance arrives or when treatment begins. It starts long before the emergency itself…..in what people know, how systems are set up, and how quickly clear decisions can be made when every minute matters.
Emergency Preparedness in Nigeria: What It Really Means
To understand why emergencies unfold the way they do and why outcomes differ so widely, it is important to first clarify what emergency preparedness actually means in healthcare.
Emergency preparedness refers to the ability of individuals, communities, and health systems to anticipate, recognise, and respond effectively to urgent health situations. It is not a single action or tool, but a chain of readiness that includes early recognition, immediate response, and rapid access to appropriate care.
According to the World Health Organization (WHO), a significant proportion of emergency-related deaths are preventable through timely first response and early intervention. This positions emergency preparedness not just as a health system concern, but as a core public health responsibility that extends beyond hospitals and professionals.
That distinction matters deeply in Nigeria, where emergencies often occur far from immediate medical care.
Why Emergency Preparedness in Nigeria Remains a Critical Gap
Once preparedness is clearly defined, the next question becomes unavoidable: why does such a wide gap still exist between what is known to save lives and what actually happens during emergencies in Nigeria?
Nigeria faces a complex mix of emergency risks. Road traffic injuries remain a leading cause of death and disability. Flooding and environmental hazards recur annually. Infectious disease outbreaks continue to pose threats. At the same time, non-communicable emergencies such as strokes, heart attacks, asthma attacks, and diabetic crises are rising steadily.
Yet emergency response capacity remains uneven.
Health system assessments consistently show that:
- The majority of emergency patients receive no organised pre-hospital care
- Ambulance availability is limited and inconsistent
- Referral pathways are often unclear
- Public understanding of emergency warning signs remains low
As a result, emergencies are frequently managed first by family members, neighbours, co-workers, or passers-by. Whether those first minutes help or harm depends almost entirely on preparedness.
This reality explains why emergency outcomes in Nigeria are shaped as much by community readiness as by hospital capacity.
First Aid Response: Where Emergency Survival Often Begins

When emergency systems are slow or stretched, the responsibility of response shifts immediately to the people present …making first aid the true starting point of emergency care.
The first few minutes after an emergency are often the most decisive. Severe bleeding, airway obstruction, poisoning, trauma, and envenomation can all worsen rapidly without early intervention.
First aid is not about replacing professional care. It is about preventing deterioration while help is being sought.
Evidence from emergency medicine research shows that simple first-aid measures such as bleeding control, correct positioning, and airway support can significantly reduce complications and mortality, particularly in settings where response times are prolonged.
As emergency care physician Dr. Yemi Adebayo explains:
“In emergencies, doing the right simple thing early is often more powerful than doing the perfect thing late.”
Despite this, access to structured first-aid training remains limited, leaving many people uncertain or hesitant when faced with real emergencies.
CPR Training in Nigeria: A Life Skill That Cannot Wait
While many emergencies involve visible injuries, some of the deadliest emergencies happen silently and cardiac arrest is one of them.
When the heart stops pumping effectively:
- Brain injury can begin within 4–6 minutes
- Survival chances decrease by 7–10% for every minute without CPR
- Immediate CPR can double or even triple survival rates
These figures are supported by decades of global emergency medicine research.
In countries where CPR training is widespread, bystander CPR occurs in a majority of cardiac arrest cases. In Nigeria, however, CPR awareness and training remain limited, and many cardiac arrest victims receive no immediate assistance before reaching professional care.
Public health researcher Professor Aisha-Bello notes:
“CPR should be treated as a basic life skill, not a specialised medical procedure. When people hesitate because they don’t know what to do, lives are lost unnecessarily.”
Basic CPR Steps for Adults (Bystander CPR)
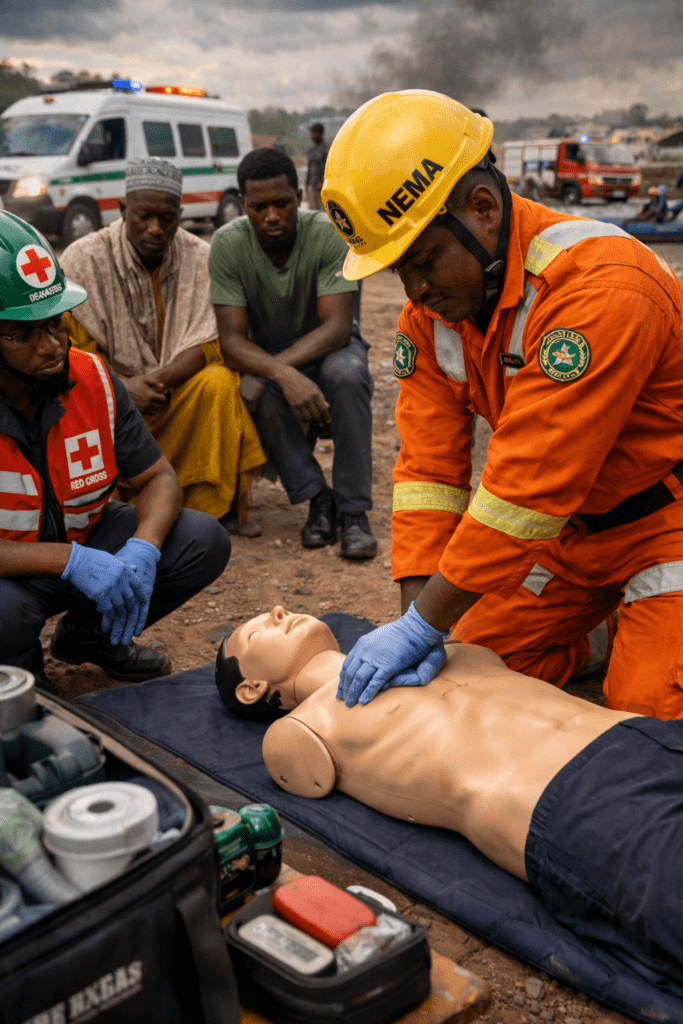
If a person suddenly collapses and is unresponsive:
- Check responsiveness and breathing
Tap the person and shout. If there is no response and no normal breathing, act immediately. - Call for emergency help
Send someone to call emergency services or seek help while CPR begins. - Start chest compressions
- Place the heel of one hand in the centre of the chest
- Place the other hand on top
- Push hard and fast at a rate of 100–120 compressions per minute
- Allow full chest recoil after each compression
- Continue until help arrives
Continue CPR until the person starts breathing, regains consciousness, or trained help takes over.
Medical evidence consistently shows that hands-only CPR is effective and far better than doing nothing.
Poisonous Snake Incidents in Nigeria Is Also An Overlooked Emergency Risk
.
Beyond cardiac and trauma emergencies, Nigeria also faces a neglected but highly time-sensitive threat….venomous snakebites, particularly in rural and agricultural communities.
Nigeria records tens of thousands of snakebite cases each year. Common venomous species include:
- Carpet vipers (Echis ocellatus), responsible for a significant proportion of fatal bites
- Puff adders
- Cobras
The World Health Organization classifies snakebite envenoming as a neglected tropical disease, largely because outcomes depend heavily on early recognition, correct first aid, and rapid access to antivenom.
First Aid Response to Snakebites (WHO-Aligned Guidance)
Snakebite envenoming is a medical emergency. The goal of first aid is to slow venom spread and ensure rapid transport to a facility with antivenom, not to attempt venom removal at the scene.
What to Do Immediately:
- Move the victim away from the snake and ensure safety
- Keep the victim calm and as still as possible
- Immobilise the bitten limb using a splint or sling
- Keep the limb at heart level or slightly below
- Remove tight clothing, rings, or jewellery before swelling begins
- Transport the victim urgently to a healthcare facility with antivenom
What NOT to Do:
- Do not cut or suck the wound
- Do not apply tourniquets
- Do not use electric shocks, ice, chemicals, or herbal remedies
- Do not delay hospital care for home treatments
Toxicology specialist Samuel Stellpflug explains that:
“Most deaths from snakebite are not caused by venom alone, but by delays, harmful first-aid practices, and lack of timely access to antivenom.”
Emergency preparedness in this context means knowing what helps and what causes harm before a bite ever happens.
From Individual Action to System Readiness
Even when individuals respond correctly, survival still depends on what happens next and that is where systems either support or fail emergency care.
Emergency preparedness in Nigeria relies on how effectively individual action connects to health systems: transport, referral pathways, trained personnel, and available supplies.
This transition from personal response to system response is where many emergencies falter.
Preparedness Isn’t Just About Medicine — It’s About Systems and People
Emergency responsiveness is not only about drugs or ambulances. It is about how systems function under pressure.
Across Nigeria and similar settings:
- Flood early-warning systems have reduced outbreaks of cholera and other water-borne diseases
- Decentralised transport solutions, including tricycle and boat ambulances, have saved lives in hard-to-reach communities
- Targeted health workforce training has improved decision-making and reduced fatal delays
Despite these gains, gaps remain.
Surveys show that:
- Only about 37% of stakeholders report functional emergency preparedness plans
- Fewer than one in four report having dedicated preparedness budgets
This gap between awareness and implementation continues to limit emergency outcomes.
Health Information Remains the Quiet Backbone of Emergency Preparedness
In emergencies, people do not analyse…. they recall.
Health information only saves lives when it is:
- Clear
- Practical
- Familiar
- Easy to remember under stress
Public health experts consistently stress that education delivered before emergencies determines behaviour during emergencies.
Technology and Emergency Preparedness in Nigeria
Digital health tools increasingly shape healthcare access. When designed with emergencies in mind, they reduce confusion and shorten decision time.
However, technology supports preparedness only when people already trust and understand it before a crisis occurs.
Access to Verified Medicines When Minutes Matter
One of the most dangerous delays during emergencies is uncertainty about where to find safe, genuine medications quickly.
For time-sensitive treatments such as antivenoms, insulin, emergency antibiotics, or antidotes….delays and counterfeit products can be fatal.
Platforms like myMedicines support emergency preparedness by:
- Improving access to verified medicines
- Reducing time lost during urgent searches
- Supporting informed, faster decision-making
Preparedness includes knowing where safe medicines come from before you need them.
Strengthening Emergency Preparedness in Nigeria
Improving emergency preparedness requires action across several fronts:
- Widespread first aid and CPR training
- Clear emergency recognition guidance
- Stronger pre-hospital and referral systems
- Technology built for speed, trust, and clarity
Why Emergency Preparedness Must Be a Public Health Priority
Emergency preparedness does not eliminate risk. It reduces loss.
In Nigeria, where emergencies are frequent and response systems are stretched, preparedness determines whether emergencies become survivable events or preventable tragedies.
When people know what to do, when systems respond quickly, and when access to care is clear, outcomes change, not by chance, but by preparation.
If this article helped you, share it.
Emergency preparedness saves lives only when knowledge spreads. Share this with your family, friends, and colleagues….because the person who needs this information tomorrow could be someone you love.
